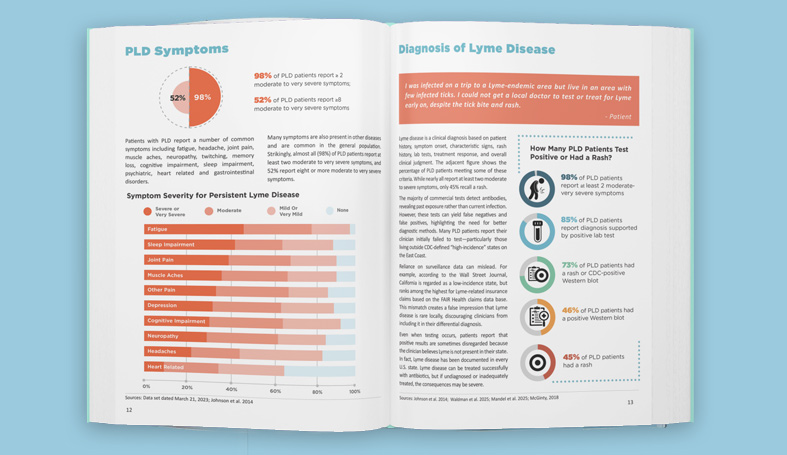
One of the thorniest issues in Lyme disease has to do with the use of antibiotics. According to the Infectious Diseases Society of America (IDSA) and Centers for Disease Control and Prevention, 2-4 weeks of antibiotic treatment is more than enough to knock out the illness.
Here’s the problem with that. Every year, tens of thousands of people who take that prescribed short course of treatment remain ill. This happens to some of those diagnosed early, and it happens more to those whose diagnosis is delayed. But the IDSA and CDC recommend no further treatment for them. They just say, “Don’t take any more antibiotics.”
Patients who still hope to recover their health often find their way to doctors willing to prescribe longer courses of antibiotics for Lyme disease. And as a result, some people get much better. Unfortunately, however, not everybody.
This is one of the questions we have sought to answer through our MyLymeData patient registry: Why do some people improve substantially with antibiotic treatment, while others do not?
Our recently published peer-reviewed study of over 2,000 participants from MyLymeData begins to answer those questions.
How do patients respond to treatment?
We looked at patients with chronic Lyme disease—those who remained ill for six or more months following treatment with antibiotics for Lyme disease (Shor 2019). The first thing we did was identify different patients as well, high responders, low responders, or non-responders. Well patients responded positively to a survey question asking if they were well or remained ill. Those who remained ill were asked whether their condition had changed as a result of treatment. Those who said they were unchanged or worse (41%) were categorized as non-responders. Patients who said that they were better or worse following treatment, were asked how much better or worse. Those who had improved substantially (moderate to a very great deal of improvement) were deemed high responders.
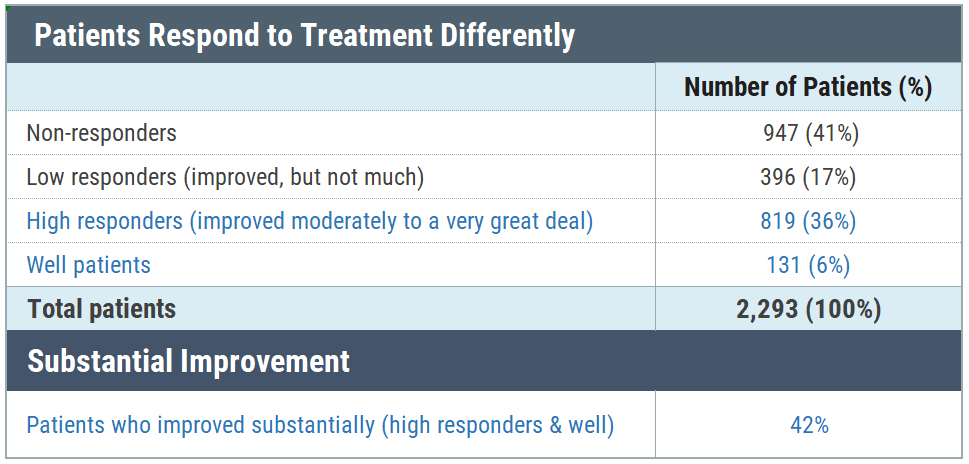
59% of patients had improved with treatment and 42% were either well or high responders. The focus of our study was on this latter group. You might wonder whether 42% response is considered good compared to other drugs. (I know I did.) Here’s what the prior head of GlaxoSmithKline said about treatment effectiveness rates of drugs in general (Connor, 2003).
“The vast majority of drugs – more than 90 per cent – only work in 30 or 50 per cent of the people. Drugs out there on the market work, but they don’t work in everybody.”
— Dr. Allen Roses, GlaxoSmithKline
So you can see that a 42% rate of substantial improvement is within the range of most drugs on the market.
Compared to the general population and patients with other chronic diseases, chronic Lyme patients report a substantially lower quality of life and a significant symptom disease burden. In this study, high responders and well patients reported substantially better quality of life, a greater percentage of improvement, and reduction in symptom severity. Patients who identified as well reported their quality of life comparable to the US general population.
What factors determine how patients respond to treatment?
To find out what made some patient substantially improve or become well, we turned to our academic partners at the University of California at Los Angeles who specialize in artificial intelligence and machine learning. Their team looked at 215 features related to diagnostic factors, treatment approach, duration of individual antibiotics, alternative treatments, symptoms, type of clinician, and functional impairment to identify the 30 top predictive features for treatment response (Vendrow 2020). Most of the top 30 features identified in their study related to chronic Lyme disease treatment (20), symptom severity (9), and type of clinician treating Lyme disease. We analyzed three of these factors associated with treatment response:
- Treatment approach (antibiotics, alternative, both or no treatment)
- Treatment durations
- Type of clinician overseeing the patients care
What treatment approach did well patients and high responders use?
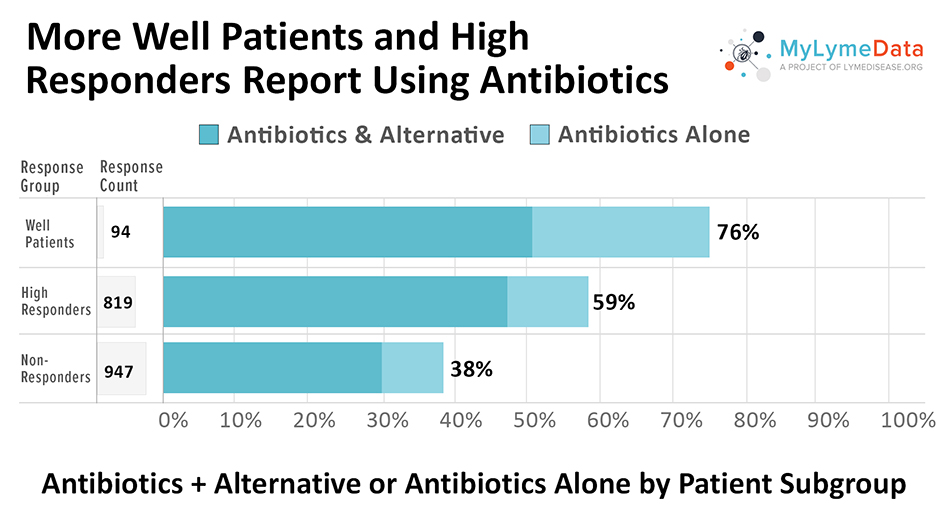
We asked patients what their treatment approach was and listed four options a) antibiotics, b) alternative treatments, c) both antibiotics and alternative treatments, and d) no treatment at all. High treatment response was most closely associated with the use of antibiotics compared to patients who were using alternative treatments alone or forgoing treatment altogether. Treatment with antibiotics for Lyme disease was far higher among well patients (76%) and high responders (59%) compared to non-responders (38%).
As you can see in the chart below, many patients who were taking antibiotics were also taking herbal supplements, which can be antimicrobial (kill bacteria and viruses). So it is possible that there was a synergistic effect between antibiotics and herbal supplements.
Why this is important
The use and duration of antibiotics for chronic Lyme disease treatment is controversial because there is no biomarker that can determine whether the Lyme bacteria has been eradicated in CLD patients. Patients are often told that either chronic Lyme disease does not exist or that it is “incurable.” If this were true, we would not expect more well and substantially improved patients to be taking antibiotics. Instead, we might have expected the percentage of people using antibiotics to be roughly the same among the patient subgroups.
Treatment duration
The optimal chronic Lyme disease treatment is unknown. The four retreatment trials by the National Institute of Health on small samples of patients have produced conflicting results—and most importantly — were all limited to 90 days of treatment (Krupp 2003, Fallon 2008, Klempner 2001, Delong 2012). The Infectious Diseases Society of America (IDSA) and the CDC generally do not recommend treatment for longer than a month (Wormser 2006).
However, a study by the CDC found that patients with Lyme disease generally reported longer treatment durations – with 60% of patients treated for five or more weeks and 36% treated for more than eight weeks (Hook 2015). Unfortunately, that study did not ask patients how long they had been ill. And, the CDC assumed these patients had acute disease – an assumption that may have been wrong. Without looking further, the CDC simply concluded that physicians needed to be better trained to shorten their treatment duration to less than a month.
But, as the chart below illustrates, in the study longer chronic Lyme disease treatment durations were common. Most were treated for four or more months (57%), and 32% were treated for more than a year.
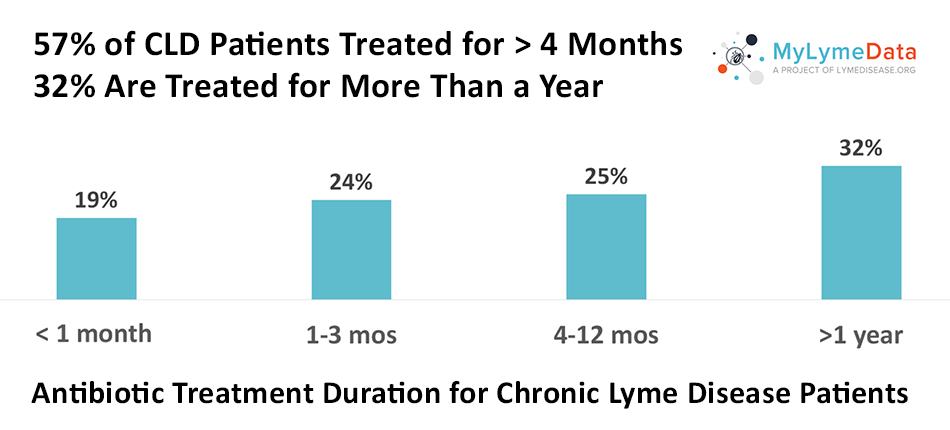
More importantly, longer treatment durations were associated with better treatment response—with most high responders and well patients reporting treatment durations of four or more months and many reported durations exceeding a year. As the chart below reveals, those treated for less than a month were unlikely to report improvement.
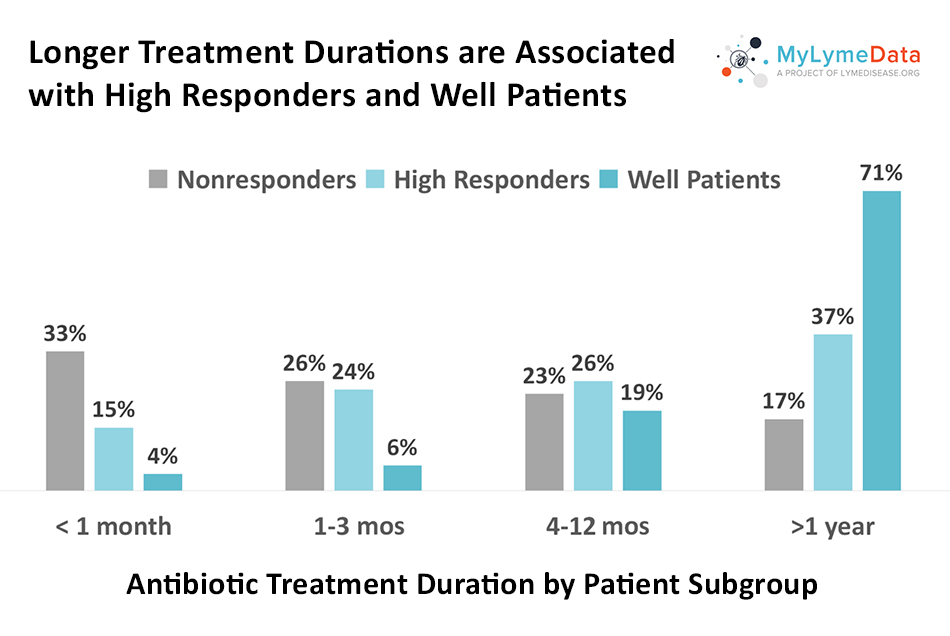
Why this is important
Insurance companies often deny payment for extended antibiotic care for Lyme disease. . Furthermore, many physicians who prescribe long-term antibiotics have been targeted by medical boards. Yet, longer treatments are seen across the board here, with 57% exceeding four months and 32% exceeding one year. This means that these lengths of treatment are common for patients with chronic Lyme disease and reflect clinical practice in the community.
As many as 3 million people have chronic Lyme disease in the US, and nobody knows the best way to treat them,” said Lorraine Johnson, CEO of LymeDisease.org. “The key finding here is that patients who are now well or who report substantial improvement have taken longer courses of antibiotics.”
The fact that more patients who are well or have substantial improvement report longer treatment durations tells us that many patients improve with longer treatment durations. This suggests that the CDC’s conclusion that better clinician training is needed to curb treatment durations is off-base. Instead, it appears that doctors are using their clinical judgement and doing what works for their individual patients. This is the approach recommended by the International Lyme and Associated Diseases Society (ILADS) (Cameron 2014).
The implications of this are profound because they suggest that the legal “standard of care” for patients with chronic Lyme disease is for longer treatment durations. When patients with the most improvement in their health report the longest treatment durations, how can you argue that it should be denied?
Type of clinician overseeing care
We asked patients to tell us the type of clinician overseeing their care. Choices included: family physicians, internists, rheumatologists, infectious disease specialists, and clinicians whose practice focused on tick-borne diseases (often referred to as Lyme Literate MDs or LLMDs). Very few patients (11%) selected an infectious disease specialist. Seventy-five percent of high responders and well patients report having their care overseen by an LLMD.
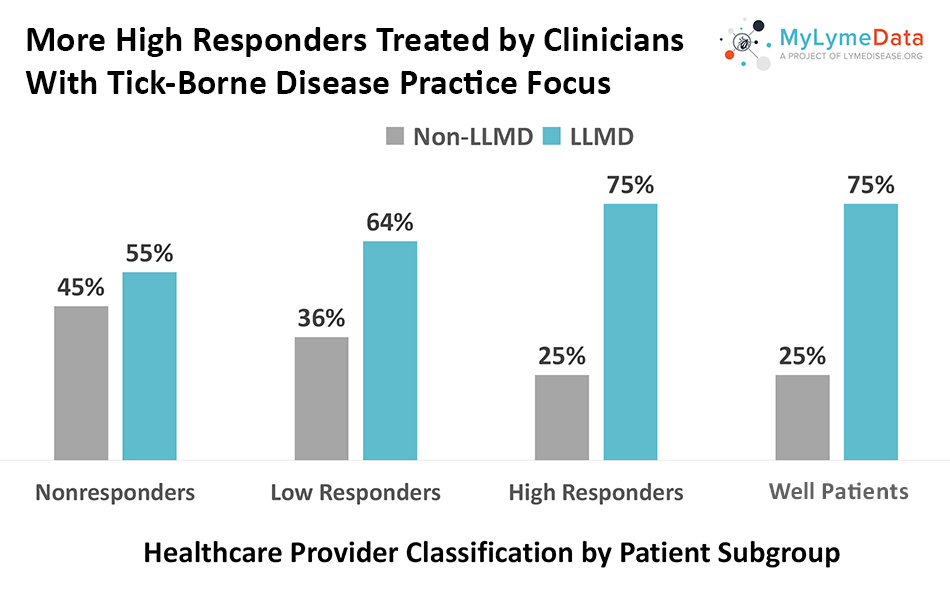
Physicians who treat Lyme disease as their primary focus might be expected to have better results than physicians who don’t simply because volume of cases handled means a greater experience level. It is commonly recognized in medicine that volume of cases is associated with better treatment outcomes (Joynt 2013). Just as patients with cancer commonly seek out physicians who specialize in that area, perhaps patients with chronic Lyme disease should also.
Why this is important
Medical boards, insurance companies, and the government often rely on the treatment guidelines of the IDSA on the basis that IDSA clinicians have the most expertise in infectious diseases and, accordingly, know what is best for patients with Lyme disease. However, patients with chronic Lyme disease are generally not treated by infectious disease experts. When short term treatment protocols fail, they find another physician to provide more individualized and longer term care. Many of these clinicians specialize in treating chronic Lyme disease and have developed greater experience and knowledge about what works. It is important that high responders and well patients more often report using LLMDs. This shows that LLMDs are associated with better patient outcomes and their expertise in this area should be more highly valued.
Main take-aways
Let me leave you with these three take-aways from the study. Chronic Lyme disease patients who improve substantially more often:
- Use antibiotics as part of their treatment approach
- Take antibiotics for more than 4 months and often for more than a year
- Rely on LLMDs to oversee their care
A note of caution: None of this should be taken to suggest that patients should blindly take antibiotics for longer durations to get well. These findings are preliminary – observational studies like this do not have control groups and cannot prove cause and effect. What they can do is suggest approaches that may improve patient outcomes. Patients vary considerably in their treatment response. In chronic Lyme disease treatment, one size does not fit all. In fact, when patients who were not taking antibiotics were ask why, about 25% responded that antibiotics had never worked for them. And some responded that antibiotics “no longer” worked for them. But for now, it seems that doctors should be using individualized care based on their diagnosis and the response of this particular patient to treatments.
The other thing this study suggests is that we have a long way to go to determine optimal care for chronic Lyme patients. For example, why do some patients not respond to treatment and which antibiotics are the most effective?
Personal Reflections
Back in 2004, when I was just beginning to get well after being ill for about five years, I co-authored a commentary with Dr. Raphael Stricker about Lyme disease having “two standards of care.” Before becoming ill, I had a robust career as a lawyer. Thus, it was natural that I would address a legal topic as my first opportunity to give back to a community that had made it possible for me to recover. But at that time, I was thinking that the two standards of care related to the divergent guidelines of the IDSA and the International Lyme and Associated Diseases Society.
With this study, it now seems that the two standards of care still exist, but that they reflect how physicians are treating different stages of the disease. People treated under the IDSA guidelines are mainly those with acute disease—the rash, Bell’s palsy, or a flu-like illness after a recent tick bite. When patients remain ill after the short courses of antibiotics offered by the IDSA, they look for clinicians who are more experienced with treating chronic Lyme disease—typically LLMDs.
A few years ago, someone asked me whether it was important to be treated by an LLMD or if they should see someone who did not focus on Lyme disease. And, although I told the person “you know, I think you might do better with an LLMD,” I had no data to back up that suggestion. Now we do.
- Cameron, D.J.; Johnson, L.B.; Maloney, E.L. Evidence assessments and guideline recommendations in Lyme disease: The clinical management of known tick bites, erythema migrans rashes and persistent disease. Expert Rev. Anti Infect. Ther. 2014, 12, 1103–1135, doi:10.1586/14787210.2014.940900.
- Connor, S. Glaxo chief: Our drugs do not work on most patients. The Indep. 2003, 8, 1–2. https://www.independent.co.uk/news/science/glaxo-chief-our-drugs-do-not-work-on-most-patients-5508670.html
- Delong, A.K.; Blossom, B.; Maloney, E.L.; Phillips, S.E. Antibiotic retreatment of Lyme disease in patients with persistent symptoms: A biostatistical review of randomized, placebo-controlled, clinical trials. Contemp. Clin. Trials 2012, 33, 1132–1142, doi:10.1016/j.cct.2012.08.009.
- Fallon, B.A.; Keilp, J.G.; Corbera, K.M.; Petkova, E.; Britton, C.B.; Dwyer, E.; Slavov, I.; Cheng, J.; Dobkin, J.; Nelson, D.R.; et al. A randomized, placebo-controlled trial of repeated IV antibiotic therapy for Lyme encephalopathy. Neurology 2008, 70, 992–1003, doi:10.1212/01.wnl.0000284604.61160.2d.
- Klempner, M.S.; Hu, L.T.; Evans, J.; Schmid, C.H.; Johnson, G.M.; Trevino, R.P.; Norton, D.; Levy, L.; Wall, D.; McCall, J.; et al. Two Controlled Trials of Antibiotic Treatment in Patients with Persistent Symptoms and a History of Lyme Disease. N. Engl. J. Med. 2001, 345, 85–92, doi:10.1056/nejm200107123450202.
- Krupp, L.B.; Hyman, L.G.; Grimson, R.; Coyle, P.K.; Melville, P.; Ahnn, S.; Dattwyler, R.; Chandler, B. Study and treatment of post Lyme disease (STOP-LD): A randomized double masked clinical trial. Neurology 2003, 60, 1923–1930, doi:10.1212/01.wnl.0000071227.23769.9e.
- Hook, S.A.; Nelson, C.A.; Mead, P.S. U.S. public’s experience with ticks and tick-borne diseases: Results from national HealthStyles surveys. Ticks Tick Borne Dis. 2015, 6, 483–488, doi:10.1016/j.ttbdis.2015.03.017.
- Johnson, L.; Shapiro, M.; Stricker, R.B.; Vendrow, J.; Haddock, J.; Needell, D. Antibiotic Treatment Response in Chronic Lyme Disease: Why Do Some Patients Improve While Others Do Not? Healthcare 2020, 8, 383. https://www.mdpi.com/2227-9032/8/4/383
- Johnson, L.; Shapiro, M.; Mankoff, J. Removing the Mask of Average Treatment Effects in Chronic Lyme Disease Research Using Big Data and Subgroup Analysis. Healthcare 2018, 6, 124, doi:10.3390/healthcare6040124.
- Johnson, L.; Aylward, A.; Stricker, R.B. Healthcare access and burden of care for patients with Lyme disease: A large United States survey. Health Policy 2011, 102, 64–71, doi:10.1016/j.healthpol.2011.05.007.
- Johnson, L.; Wilcox, S.; Mankoff, J.; Stricker, R.B. Severity of chronic Lyme disease compared to other chronic conditions: A quality of life survey. PeerJ 2014, 2, e322, doi:10.7717/peerj.322.
- Joynt, K.E.; Orav, E.J.; Jha, A.K. Physician Volume, Specialty, and Outcomes of Care for Patients With Heart Failure. Circ. Hear. Fail. 2013, 6, 890–897, doi:10.1161/circheartfailure.112.000064.
- Shor, S.; Green, C.; Szantyr, B.; Phillips, S.; Liegner, K.; Burrascano, J.J., Jr.; Bransfield, R.C.; Maloney, E.L. Chronic Lyme Disease: An Evidence-Based Definition by the ILADS Working Group. Antibiotics 2019, 8, 269, doi:10.3390/antibiotics8040269.
- Vendrow, J.; Haddock, J.; Needell, D.; Johnson, L. Feature Selection on Lyme Disease Patient Survey Data. arXiv Prepr. 2020, arXiv:2009.09087.
- Wormser, G.P.; Dattwyler, R.J.; Shapiro, E.D.; Halperin, J.J.; Steere, A.C.; Klempner, M.S.; Krause, P.J.; Bakken, J.S.; Strle, F.; Stanek, G.; et al. The Clinical Assessment, Treatment, and Prevention of Lyme Disease, Human Granulocytic Anaplasmosis, and Babesiosis: Clinical Practice Guidelines by the Infectious Diseases Society of America. Clin. Infect. Dis. 2006, 43, 1089–1134, doi:10.1086/508667.
If you are a patient who is not enrolled in MyLymeData, please enroll today. If you are a researcher who wants to collaborate with us, please contact me directly.
The MyLymeData Viz Blog is written by Lorraine Johnson, JD, MBA, who is the Chief Executive Officer of LymeDisease.org. You can contact her at lbjohnson@lymedisease.org. On Twitter, follow her @lymepolicywonk.