LYMEPOLICYWONK: Growing Number Of Chronic Lyme Patients—Still No Government Action Plan?

Have you ever wondered how many people have chronic Lyme disease? The NIH estimates between 10-20% of those who get Lyme develop persisting symptoms. Other studies suggest between 35%-50%, depending on whether the patients had early or late Lyme disease at the time of treatment. What gives?
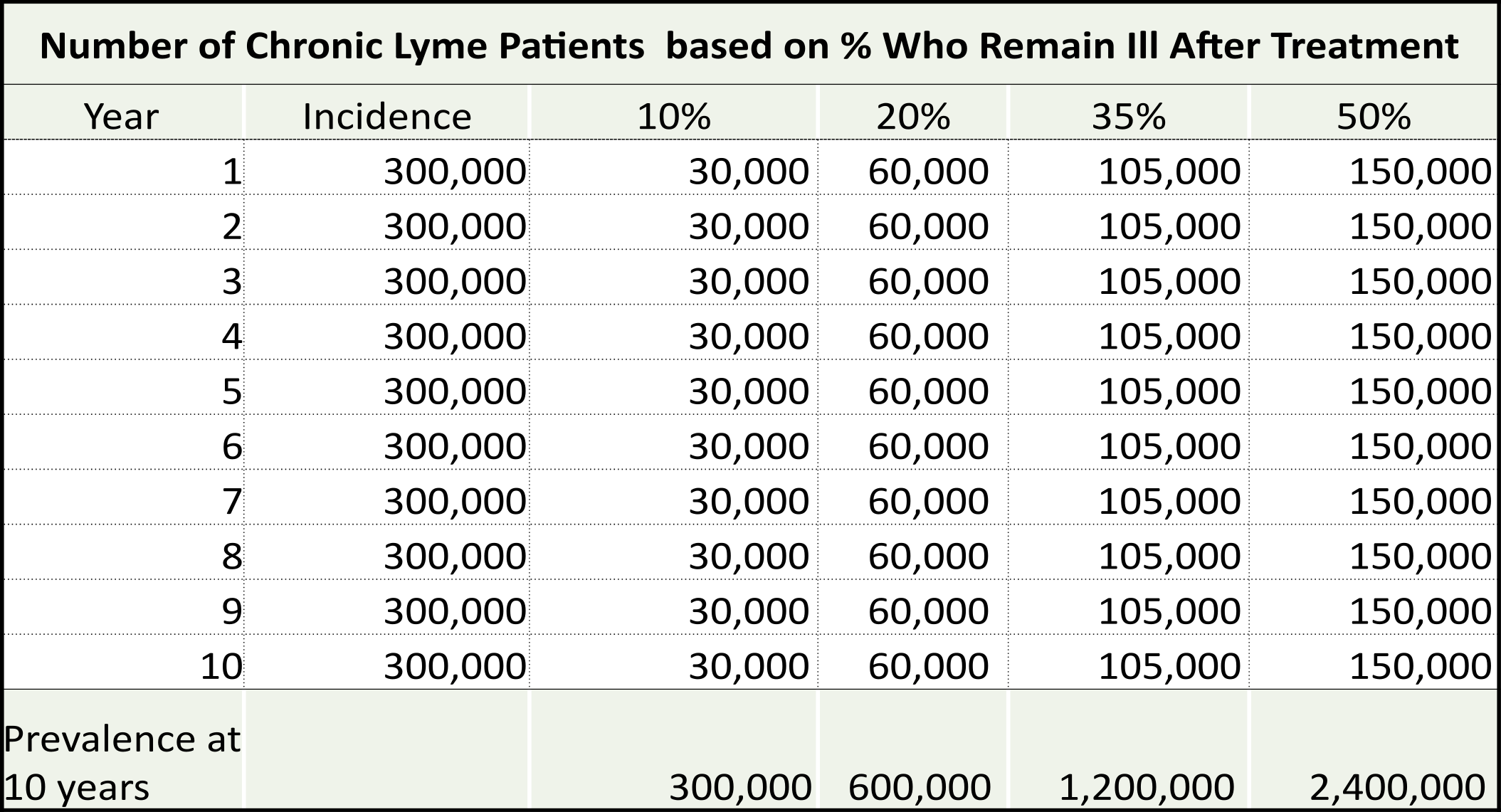
When we talk about how many people have a disease, it is important to distinguish between incidence and prevalence. Incidence is the number of people who contract Lyme disease in any given year. The recent studies by the CDC suggest this number is 300,000 and possibly as high as 420,000 a year. Many of these people will be diagnosed early and treated successfully. Those who aren’t remain ill and add to a growing burden of disease as their numbers continue to mount.
The number of people who get a disease and remain ill is what is called the disease “prevalence”. Some percentage will be diagnosed early and treated but will continue to remain ill. In addition, people who are diagnosed later are more difficult to treat and more of these remain ill. Both groups increase the prevalence of Lyme disease.
A study by Dr. Aucott at Johns Hopkins looked at patients diagnosed and treated early. He found roughly 35% remained ill. Seven other studies have found that between 27% and 50% of patients remain ill. The CDC/NIH estimates that the percentage remaining ill is between 10-20%.
So estimates range from 10-50%. Why the big difference? The differences are likely the result of what measure of success is used. Some studies measure success based on whether objective findings, like a swollen knee or a rash is resolved. Others actually consider whether the patient continues to have symptoms or is restored to wellness and able to get on with their life. Patients care about whether they get well period. Resolution of an objective finding is meaningless if you can’t work.
Anyway you cut it, the rising number of chronic Lyme disease cases is spiraling out of control and the government has no plan to address this looming problem. The table below, of course, does not reflect undiagnosed cases. Most chronic Lyme patient report in our surveys that it has taken them two years or more to achieve a diagnosis. The most obvious solution is to prevent chronic Lyme disease by insuring early diagnosis and adequate treatment to cure. The 35% treatment failure rate cited by Aucott is unacceptable. Longer treatment or treatments using a combination of treatments, as is done in Tuberculosis, would be a start to address the problem.
The LYME POLICY WONK blog is written by Lorraine Johnson, JD, MBA, who is the Chief Executive Officer of LymeDisease.org.You can contact her at lbjohnson@lymedisease.org. On Twitter, follow her @lymepolicywonk.
Bibliography:
Asch, E. S., D. I. Bujak, et al. (1994). “Lyme disease: an infectious and postinfectious syndrome.” J Rheumatol 21(3): 454-461.
Aucott, J. N., A. W. Rebman, et al. (2013). “Post-treatment Lyme disease syndrome symptomatology and the impact on life functioning: is there something here?” Qual Life Res 22(1): 75-84.
Johnson, L., S. Wilcox, et al. (2014) “Severity of chronic Lyme disease compared to other chronic conditions: a quality of life survey.” PeerJ 2, e322 DOI: 10.7717/peerj.322.
Logigian, E. L., R. F. Kaplan, et al. (1990) “Chronic neurologic manifestations of Lyme disease.” N Engl J Med 323, 1438-1444.
Pfister, H. W., V. Preac-Mursic, et al. (1991). “Randomized comparison of ceftriaxone and cefotaxime in Lyme neuroborreliosis.” J Infect Dis 163(2): 311-318.
Shadick, N. A., C. B. Phillips, et al. (1994) “The long-term clinical outcomes of Lyme disease. A population-based retrospective cohort study.” Ann Intern Med 121, 560-567.
Shadick, N. A., C. B. Phillips, et al. (1999). “Musculoskeletal and neurologic outcomes in patients with previously treated Lyme disease.” Ann Intern Med 131(12): 919-926.
Treib, J., A. Fernandez, et al. (1998). “Clinical and serologic follow-up in patients with neuroborreliosis.” Neurology 51(5): 1489-1491.
Valesova, H., J. Mailer, et al. (1996). “Long-term results in patients with Lyme arthritis following treatment with ceftriaxone.” Infection 24(1): 98-102.




















lorraine, thank you for the above info galore.
i love how you and dorothy are coming out DAILY providing new info/articles/studies done so we can be aware of them.
KUDOS to lorraine and dorothy! 😉
bettyg, iowa lyme activist
46.5 yrs. chronic lyme
35 yrs. MISDIAGNOSED by 40-50 drs.
UNACCEPTABLE!
lorraine, thank you for the above info galore.
i love how you and dorothy are coming out DAILY providing new info/articles/studies done so we can be aware of them.
KUDOS to lorraine and dorothy! 😉
bettyg, iowa lyme activist
46.5 yrs. chronic lyme
35 yrs. MISDIAGNOSED by 40-50 drs.
UNACCEPTABLE!
What is occurring is a crime against humanity.
I never expected this barbaric behavior of the medical field, the cdc, nih.
Those not enduring this or have a close relationship with someone with chronic lyme disease have no idea the torture in which we live and the way we are made to seem crazy, ridiculed, not helped, left undiagnosed…
I am undiagnosed, too ill to work, no health insurance, no income, lost my home yet I have no doc to diagnose me and help me get disability either.
I have only tears. http://www.caringbridge.org/visit/slippingaway
marcie, i posted just now on your caring bridge site. so please read my message over there. i’ll help you all i can with the knowledge/experience i have.
bettyg, iowa lyme activist
46.5 yrs. chronic lyme
35 yrs. MISDIAGNOSED by 40-50 drs;
UNACCEPTABLE!
Marcie, I’ve been unable to work for over two years. I’ve had to go on Medicaid and food stamps, sold some belongings, and am $20k in debt from medical expenses. It’s a horrible situation.
Please get in touch with your state or county’s social services dept. You need Medicaid and food stamps asap.
Another great article from Lorraine Johnson. How long will the turning the blind eye last? Thanks Lorraine for your work!
I am 43 lyme showed on my blood work finally after being sick for 3 years and still they will not say its lyme disease they say neurological issues i can not work no insurance as of the end of this month and no income staying with friends. Dont know what to do
There are too many of us in this predictament. It is wrong, inhumane and barbaric to be treated like this, shunned from those you seek help, left to lose everything while getting more and more ill and you can’t even think well enough to figure any of it out any more.
This is a crime against humanity.
My estimate, based on my observations here in CT, is that 9 out of ten Lyme sufferers are misdiagnosed, and have been for years. Consequently, if the number of diagnosed cases is 300,000 per year, it is likely that the true number of new cases is 3 million a year. The prevalence could very well be in the tens of millions.
Looking at just my own (extended) family: ten individuals have symptoms of chronic Lyme. Of these ten, only one – me – has a Lyme diagnosis and getting treatment. Two others were diagnosed and treated for acute Lyme years ago. Both still have life-altering symptoms, one has become a borderline psychotic recluse. Two others have many psych and physical symptoms and eventually tested IGENEX positive but never got treatment. One other I believe died of the disease, after decades suffering from “epilepsy”, schizo-affective disorder, swallowing problems, and “Parkinson’s”. Another developed bi-polar psychosis in middle age. One other was tested for babesia, was positive, but never had a Lyme test due to insurance issues and was never treated for any tick-borne disease. I could go on and on……………..
Its people like you that can make a difference by just opening your mouth and making sure people know, I too am the same, the CDC of course dont think like we do, until of course one of them end up contracting it, thanks for your efforts, have a great day