The Bartonella clue hidden in plain sight
By Terri McCormick
What if anxiety, rage, or sudden personality changes were not purely psychiatric?
What if, in some cases, the root cause was an infection — and the body was leaving a physical clue on the skin that most people never recognize?
For more than a century, medicine has recognized that infections can affect the brain. In 1913, researchers demonstrated that the bacterial cause of syphilis could cross the blood-brain barrier and cause profound psychiatric symptoms.
Today, physicians still routinely screen for syphilis when a patient presents with hallucinations, cognitive decline, or sudden behavioral changes.
But here is the strange part. Doctors continue to look for a 100-year-old infection while often overlooking modern-day pathogens that can do the very same thing.
Among them is Bartonella, an elusive bacterium carried by ticks, fleas, lice, cats, and other animals. According to Dr. Edward Breitschwerdt, one of the world’s leading Bartonella experts, very few studies have examined the skin changes linked to Bartonella.
That lack of research may help explain why these markings are so often ignored, even when they appear alongside significant neuropsychiatric symptoms.
 The rash no one is looking at
The rash no one is looking at
One of the most overlooked clues may be right on the skin.
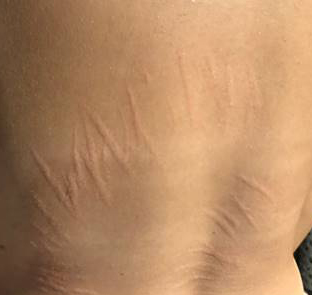
Across several studies, patients with neuropsychiatric symptoms such as anxiety, depression, rage episodes, OCD-like behaviors, and hallucinations have been found to develop unusual lesions that look like stretch marks. But they aren’t stretch marks.
They often appear in unusual locations, occur without significant growth or weight gain, and develop at the same time psychiatric symptoms begin.
Not every patient develops these markings, but when present, they may offer an important clinical clue. Several published studies have described Bartonella-associated skin lesions in patients with neuropsychiatric symptoms.¹
Yet Bartonella-associated skin lesions are not currently recognized by the American Academy of Dermatology and are not listed as a distinct clinical finding within its educational materials. As a result, these markings are frequently dismissed as cosmetic stretch marks, even when they do not behave like stretch marks at all.
When a rash is dismissed, a valuable diagnostic clue may be lost. If someone has psychiatric symptoms and an unexplained rash that looks like stretch marks, that is a signal worth investigating, not ignoring.
Tick-borne infections and the brain
The connection between infection and psychiatric symptoms is supported by a growing body of research.
Tick-borne infections, including Lyme disease, Bartonella, and Babesia, have been linked to such symptoms as anxiety, depression, panic attacks, irritability and rage, cognitive impairment, derealization, hallucinations, OCD-like behaviors, sudden personality changes, and even psychosis.
These patterns have been reported in peer-reviewed literature, including case reports, and increasingly in larger studies. Even so, many clinicians are not routinely trained to consider infections when evaluating psychiatric symptoms. Instead, treatment often focuses on managing behaviors without exploring what might be driving those changes in the first place.
Two rising curves
As research continues to reveal the overlap between tick, flea and other vector-borne infections and psychiatric symptoms, a broader question begins to emerge.
Is there a relationship between the rise in psychiatric illness and the rise in vector-borne infections?
Each year, hundreds of thousands of people in the United States are diagnosed with Lyme and other tick-borne diseases, and experts believe the true number is even higher. At the same time, rates of anxiety, depression, OCD, and other psychiatric conditions continue to climb.
Correlation does not prove causation, but it can point to areas that deserve closer attention. When similar patterns appear across patient experiences and emerging research, it raises an important question. Are we looking closely enough?
As powerful as the research is, the impact becomes even clearer when you look at what happens in real lives. One of those stories is Kurt’s, a middle-aged man whose mental health had declined in recent years.
A missed clue, found
Kurt had spent nearly a decade searching for answers. Over the years, he saw multiple physicians as his symptoms worsened. His personality changed, and cognitive issues emerged. He received several diagnoses, including early-onset Alzheimer’s disease.
Nothing fully explained what was happening.
Kurt eventually became a client of Lisa Selenko, PhD, CGT, a Gestalt psychotherapist with knowledge of tick-borne infections. She asked him a simple question she asks many of her clients: had he noticed any unusual changes on his skin?
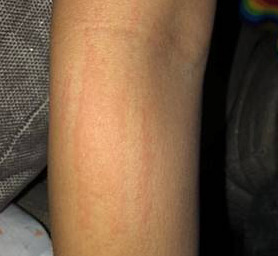
Kurt had long, streak-like markings on his stomach that had been dismissed for years as ordinary stretch marks. No one had ever connected them to his symptoms.
Selenko took this detail seriously. When she considered the markings alongside his neuropsychiatric symptoms, she suspected more might be going on. She referred him to a physician with advanced training in complex chronic illness and tick-borne disease.
There, he was evaluated and ultimately treated for Bartonella and Lyme disease.
Kurt credits Selenko with helping uncover the root of his illness and changing the course of his life. With treatment, his symptoms began to improve. His thinking became clearer, his personality stabilized, and over time, even the markings that had once been dismissed began to fade.
Understanding the limits of the model
Selenko is quick to point out that mental health professionals operate within a system that shapes how they think.
“Mental health professionals are trained to rely on the DSM (Diagnostic and Statistical Manual of Mental Disorders) as a structured framework for diagnosing mental health issues. At the same time, most insurance companies require a formal DSM diagnosis to cover therapy. This system naturally pushes clinicians toward labeling symptoms within mental health categories, even when the root cause may lie elsewhere.”
While the DSM acknowledges that medical conditions, including chronic infections, can contribute to psychiatric symptoms, it is primarily designed to classify symptom patterns—not to investigate or identify their underlying causes.
Selenko’s approach does not reject this model. Rather, it expands upon it by asking different questions and paying attention to patterns and medical conditions that might otherwise be overlooked.
Her approach reflects something simple but often missing in clinical care. It is not only about assigning a diagnosis and managing symptoms. It is about looking carefully at the person in front of you and asking whether something else could be contributing.
For some patients, that shift in perspective can make all the difference.
What this means for patients
If you or someone you love is experiencing psychiatric symptoms that do not fully make sense, it may be worth asking additional questions.
Are there unexplained physical symptoms, changes in the skin, or signs that something more may be going on? Could an underlying infection be part of the picture?
Vector-borne illnesses, including Lyme disease and Bartonella, can show up in ways that are not always immediately recognized. While testing can support a diagnosis, results may not always capture the full picture, making careful clinical evaluation essential.
For this reason, it can be important to seek out clinicians with advanced training in tick-borne disease who are experienced in evaluating complex, multi-system illness.
This is not about replacing psychiatric care. It is about expanding the lens so that nothing important gets overlooked.
Because sometimes, asking the right questions can change the course of a patient’s life.
Terri McCormick is a writer and advocate with LymeDisease.org. She is the author of the forthcoming book Being Misdiagnosed: Stories That Reveal the Hidden Epidemic of Lyme Disease, releasing May 1 in honor of Lyme Disease Awareness Month. Pre-order at TerriMcCormick.com.
References
- Breitschwerdt EB, Bradley JM, Maggi RG, et al. Bartonella-associated cutaneous lesions (BACL) in people with neuropsychiatric symptoms. Pathogens. 2020;9(12):1023.
- Stewart Z, Korsapathy S, Frohlich F. Crowd-sourced investigation of a potential relationship between Bartonella-associated cutaneous lesions and neuropsychiatric symptoms. Front Psychiatry. 2023;14:1244121.
- Breitschwerdt EB, Greenberg R, Maggi RG, et al. Bartonella henselae bloodstream infection in a boy with pediatric acute-onset neuropsychiatric syndrome. J Cent Nerv Syst Dis. 2019;11:1–8.
- Breitschwerdt EB, Maggi RG, Robveille C, et al. Bartonella henselae, Babesia odocoilei and Babesia divergens-like MO-1 infection in the brain of a child with seizures. J Cent Nerv Syst Dis. 2025;17:1–10.
- Breitschwerdt EB, Maggi RG, Bush JC, et al. Babesia and Bartonella species DNA in blood and enrichment cultures from people with chronic fatigue and neurological symptoms. Pathogens. 2025;15:2.
- Heymann WR. Striae due to Bartonella is a stretch. Dermatology World Insights and Inquiries. American Academy of Dermatology. 2018.
- Bransfield RC. Microbes and mental illness: past, present, and future. Psychiatr Clin North Am. 2017;40(3):419–438.














 The rash no one is looking at
The rash no one is looking at





We invite you to comment on our Facebook page.
Visit LymeDisease.org Facebook Page