Genes and Environment Trigger New Chronic Illnesses Dr. Neil Nathan's book, "Toxic" seeks to help "ultrasensitive” patients with mold toxicity, Lyme disease, multiple chemical sensitivities, and chronic environmental illness.
W hen Dr. Nathan started treating patients 50 years ago, the model for medicine was much simpler—a standard diagnosis followed by a standard treatment. Now, he says, “The patients who come to see me today are a quantum leap (or two) sicker than the ones who came to me in the late 1980s.”

Today’s patients are sicker, for longer, with a multitude of chronic ailments that weren’t known to exist years ago. From autism to fibromyalgia to myalgic encephalomyelitis to mold toxicity—gone are the days of “take two aspirin and call me in the morning.”
As Professor Robert Naviaux, MD, a world-renowned biomedical/genetics researcher, explains in his introduction, “These new chronic illnesses have both genetic and environmental causes. They are ‘ecogenetic’ diseases that occur because the chemistry of the environment is changing faster than our genes can adapt.”
Dr. Nathan recounts the evolution of his own medical practice, progressively taking on more and more patients with whom no one else knew what to do. Now, 70% or more of his patients are classified as “ultrasensitive,” meaning they react intensely to even minuscule exposure to medications and supplements.
The topics covered in the book are straight out of Dr. Nathan’s real-world experience. While reading the book, I felt like someone was sharing with me all of their family’s secret recipes. This book is full of hard-earned knowledge. It’s a clear road map that combines the art and science of treating the sickest of the sick.
The book is organized in a way that makes it easy to return to time and time again. For instance, Chapters 8–20 provide a step-by-step guide on how to “reboot” every system of the body, arranged in the order in which they occur most frequently. So, whether you need to reset anything from your brain to your gut, it’s in there.
Understanding Mold Toxicity
TOXIC also provides one of the easiest to understand and simplest methods for identifying and treating mold toxicity that I have ever read. Dr. Nathan explains how to identify the different types of mycotoxins (mold) and then clearly lays out a four-step process for treatment.
There is also an appendix devoted to troubleshooting mold toxicity issues for highly sensitive patients and a supplement guide.
I was especially interested in the contributions by Dr. Lawrence Afrin, one of the pioneers in mast cell research. I am forever grateful for his guidance and connecting me to the right specialists, which led to my own child’s diagnosis of mast cell activation syndrome. Dr. Nathan estimates that 50% of his ultra-sensitive patients have a mast cell activation component to their illness.
The book is organized in a way that makes it easy to return to time and time again. For instance, Chapters 8–20 provide a step-by-step guide on how to “reboot” every system of the body, arranged in the order in which they occur most frequently. So, whether you need to reset anything from your brain to your gut, it’s in there.
The chapters on the cell danger response and genetics are incredibly detailed and precise and serve as proof of the science behind these complex illnesses.
Methylation
The chapter on methylation is a gift—believe me! This is one of the most poorly understood concepts in functional medicine today. No one understands this better than Dr. Nathan—he pioneered the first study on using a “simplified methylation protocol” in 2007. If taking vitamin B12 or folate makes you feel worse, you need to read this chapter!
If you’ve tried conventional treatment for Lyme disease, Bartonella, or mold yet continue to suffer from poor concentration, anxiety, headaches, insomnia, pain, ringing in the ears, strange sensations, increasing allergies to medication or food intolerance, and/or sensitivity to chemicals, you will find useful information in this book.

Dr. Nathan has been board-certified in family practice and pain management, is a founding diplomate of the American Board of Integrative Holistic Medicine, and is a board member of the International Society for Environmentally Acquired Illness (ISEAI). He recently retired from private practice after 50 years of seeing patients.
Dr. Nathan has lectured to medical audiences both nationally and internationally. He has written several books and has hosted an internationally syndicated radio program/podcast, The Cutting Edge of Health and Wellness Today.
Author: Dr. Neil Nathan
The topics covered in the book are straight out of Dr. Nathan’s real-world experience. While reading the book, I felt like someone was sharing with me all of their family’s secret recipes. This book is full of hard-earned knowledge. It’s a clear road map that combines the art and science of treating the sickest of the sick.
An excerpt from Dr. Neil Nathan’s book
TOXIC
While methylation is an important component of health and a common problem for patients suffering from chronic illnesses, it has been receiving an unusual amount of attention lately, elevating its importance to heights that are, perhaps, out of proportion to the role that it plays. I am devoting a chapter to methylation in the hope that I can help put the whole concept into perspective
What Is Methylation?
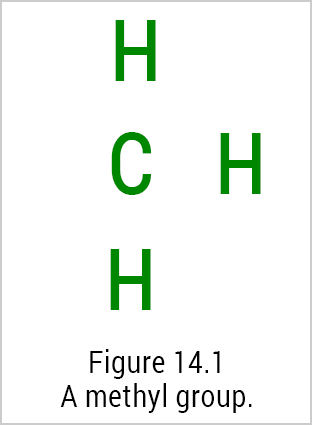
While it may sound complicated, methylation is simply the biochemical process of adding a methyl group to a molecule. A methyl group consists of a carbon atom surrounded on three sides by hydrogen atoms, allowing the fourth side (to the left of the central carbon atom in Figure 14.1) to bind to another substance.
The process of methylation is basic to hundreds of important biochemical reactions in the body. The most important of these is creating glutathione, which is a central material in creating energy, detoxifying, and dealing with free radical buildup. The body uses methylation itself for detoxifying, repairing damaged DNA, converting serotonin to melatonin, and many other critical processes.
The most common symptoms of methylation deficiency, or an inability to methylate properly, are fatigue, cognitive impairment, pain, and insomnia.
Let’s begin with a little history of how methylation rose to the top of the to-do lists of functional medicine physicians.
How Methylation Came to Prominence

Rich Van Konynenburg, PhD, spent his career as a pioneering engineer who became a major troubleshooter for the Livermore National Laboratory. After his retirement, he became fascinated by the difficulties faced by patients with myalgic encephalopathy/chronic fatigue syndrome (ME/CFS) and fibromyalgia. He spent several years researching the biochemistry of these illnesses, and in 2003 he wrote a seminal paper suggesting that methylation chemistry, when not functioning properly, could explain virtually all of the clinical findings in ME/CFS.

This hypothesis was developed from the work of Amy Yasko, PhD, who was working with autistic children. Dr. Yasko suggested that autism was the form that illness took in younger patients and was similar to ME/CFS and fibromyalgia in adults and to neurodegenerative diseases in older patients.
Dr. Van Konynenburg was still having trouble convincing physicians to take his work seriously when I heard him speak at a medical meeting in 2007. I was so intrigued by the logic and simplicity of his ideas that when I got home from the meeting, I immediately placed fifty-one patients with ME/CFS and fibromyalgia on the five supplements that Dr. Van Konynenburg had developed from Dr. Yasko’s work and that he described as a “simplified methylation protocol.” Essentially, this protocol consisted of hydroxocobalamin (hydroxy-B12), a tiny dose of 5-methyltetrahydrofolate (5-MTHF), and several other supplements to support methylation chemistry.
After several months of taking these supplements, 70 percent of my patients noted definite improvements, and 20 percent reported that they felt markedly better.
This was the first time that Dr. Van Konynenburg’s hypothesis had been tested, and he was delighted with our initial results.

Dr. Van Konynenburg and I were fortunate to receive private funding for a more elaborate clinical study, and we entered thirty patients, all of whom met the criteria for ME/CFS and fibromyalgia, into a research project in which we measured their methylation chemistry and kept a detailed clinical symptom diary before giving them supplements. We gave all of them exactly the same supplements I had used in the pilot project and followed their clinical progress closely for nine months, measuring their methylation chemistry with a blood test from Health Diagnostic Laboratory every three months. The results were impressive. Despite the unusually long trial period, almost all of the patients participated for the entire duration.
Not a single patient who began the study had normal methylation chemistry, suggesting that Dr. Van Konynenburg’s hypothesis about abnormal methylation chemistry playing a significant role in ME/CFS and fibromyalgia was valid.
By the end of six months, glutathione and SAM had risen to normal levels in almost every patient. After nine months, they were better still. More important, the patients had improved clinically: 77 percent reported improved energy, 65 percent reported improved sleep, 73 percent reported improved mental clarity, and 54 percent reported a decrease in pain. To put this differently, 83 percent told me that they had improved (defined by them as being 15 to 50 percent better), and of those who had improved, 27 percent reported that they were much better, defined as 50 to 100 percent better. The average improvement at six months was 48 percent and was statistically significant.
Dr. Van Konynenburg and I felt that we had begun to address the important questions: Does methylation play a role in ME/CFS and fibromyalgia, and if so, Is it treatable? The answer to both questions was a resounding yes!
The funding for this project did not, by design, include an institutional review board, which would have allowed us to submit these findings to a peer-reviewed journal. You can find the details in my book Healing Is Possible and in the December 2011 issue of the Townsend Letter.
Dr. Van Konynenburg and I presented this work at quite a few medical meetings, both national and international, and it received a good deal of attention. What followed was an explosion of interest in methylation as an important component of health and illness, and it came to be viewed as a central area that needed to be addressed clinically. After all, the end product of methylation, as I have emphasized, is glutathione, which is essential for energy, detoxification, and oxidative chemistry. So methylation appears to be something that needs to be addressed early on in treatment, perhaps for everyone who is chronically ill.
Well, yes and no. As you might expect, in complex patients, it is more complicated than that.
Timing Methylation Treatment Correctly
In Chapter 8, I discussed the cell danger response (CDR). One important component of the CDR is that when a cell feels threatened, it intentionally shuts down methylation to deprive an infecting microbe of the capability to hijack the body’s own methylation chemistry so that the microbe can reproduce. It therefore should come as no surprise that virtually all chronically ill and inflamed patients, in whom the CDR has been triggered, have measurably low methylation chemistry. But does that mean we should immediately provide all patients with the supplements to maximize methylation?
It turns out that the answer to that question is: It’s all about timing.
Because the CDR is a protective mechanism, overriding that mechanism before the body is ready to move forward might not be a great idea, especially for sensitive patients. In my experience, approximately half of sensitive patients, if given vitamin B12 or folate (usually in the form of 5-MTHF), experience an intense worsening of their symptoms — even when given minuscule doses. I would like to emphasize that in our study of thirty patients, supplementing with only 200 micrograms of 5-MTHF improved every patient’s ability to methylate. Some practitioners are recommending massive dosages of folate with the idea that if some is good, more is better. This is rarely true. In my practice, in fact, the opposite is far more common. Many of the patients who come to see me are on dosages of folate that are way too high, and they improve when we reduce the dosage dramatically or stop the supplement altogether.
I have found that once a patient has eased into treatment of the underlying main issue (usually mold toxicity or Lyme disease), he or she can take methylation supplements comfortably and with benefit later in the course of treatment.
Unfortunately, some practitioners insist that because methylation is so important, especially to detoxification, patients must continue taking the supplements. Worse, they advise increasing the dosage even when a patient is clearly reacting badly. This is not wise. The vast majority of these patients will get worse — often much worse. The body is saying that it is not yet ready to begin this area of treatment.
I have found, however, that once a patient has eased into treatment of the underlying main issue (usually mold toxicity or Lyme disease), he or she can take methylation supplements comfortably and with benefit later in the course of treatment.
I worry that healthcare providers have escalated the importance of methylation in detoxification to the point that they are telling patients that if they can’t methylate, they can’t get better, so they have to keep taking their methylation supplements no matter how bad they feel.
Not so! Please keep in mind that the body has many avenues and organs of detoxification, so if methylation can’t be started early on, the body can and does utilize other systems to detoxify. Sensitive patients who cannot take methylation supplements yet can begin treatment, improve, and then initiate efforts to methylate better.
Another area I would like to address is the love affair that integrative practitioners are having with glutathione supplementation. While there is no question that glutathione is an essential component of health, its indiscriminate use is not always justified.
Many patients with mold toxicity, for example, get worse when given glutathione in any form: oral, IV, or topical. You may recall that in Chapter 3, I encouraged the use of oral glutathione as a prevocational agent to make urine testing for mycotoxins more accurate. At the same time, I cautioned that in sensitive patients, glutathione mobilizes molds (and other toxins) faster than their bodies can process those toxins, and the patients become more toxic. They experience this increase in toxicity as an intense exacerbation of their usual symptoms. This is not a reaction that these patients can override by pushing themselves to “ride it out,” although many of them try anyway. It is important to recognize when this adverse reaction is occurring and to stop taking glutathione until the body is able to right itself.
Many of my sensitive patients simply cannot take glutathione in any form until later in treatment when they are on the mend.
A second concern I have is that many practitioners do not seem to realize that glutathione, as important as it is, is carefully monitored and regulated by the body. When glutathione is taken in any form, the body’s biofeedback systems announce that it has plenty of glutathione on board now, so it can stop making glutathione using the process of methylation. What this means is that many patients who are taking glutathione are unwittingly turning off their ability to methylate, which is counterproductive in patients who already are not methylating well.

This is not to say that glutathione should not be used in treatment, but it is a plea to practitioners to make an effort to discern which patients might benefit from the use of glutathione and which should not be offered glutathione until they have improved. I have intentionally emphasized difficulties with methylation and the use of glutathione because these difficulties are common in my sensitive patients. I also want to make it clear that the use of glutathione in patients who have a stronger constitution can be quite helpful.
Janette Hope, MD, has described the use of intranasal glutathione being of great help in treating patients with mold toxicity. Many patients have found immediate and clear benefits from the use of oral or intravenous glutathione as well. My take-home message is simply to alert practitioners and patients to the possible downside of the use of glutathione and to advise you to be very careful when instituting treatment with this material.
The bottom line is that sensitive and toxic patients must approach methylation very carefully, and they and their healthcare practitioners must be mindful that this area of treatment may need to be postponed until they have begun to improve. While I believe that methylation is indeed important (heck, I helped put it on the map!), I urge patients and physicians to put its value into perspective and to always look for the greater context in which we view treatment.
From TOXIC: Heal Your Body from Mold Toxicity, Lyme Disease, Multiple Chemical Sensitivities, and Chronic Environmental Illness. Copyright © 2018 by Neil Nathan. Reprinted with permission from Victory Belt Publishing Inc.
Editor’s note: Any medical information included is based on a personal experience. For questions or concerns regarding health, please consult a doctor or medical professional.